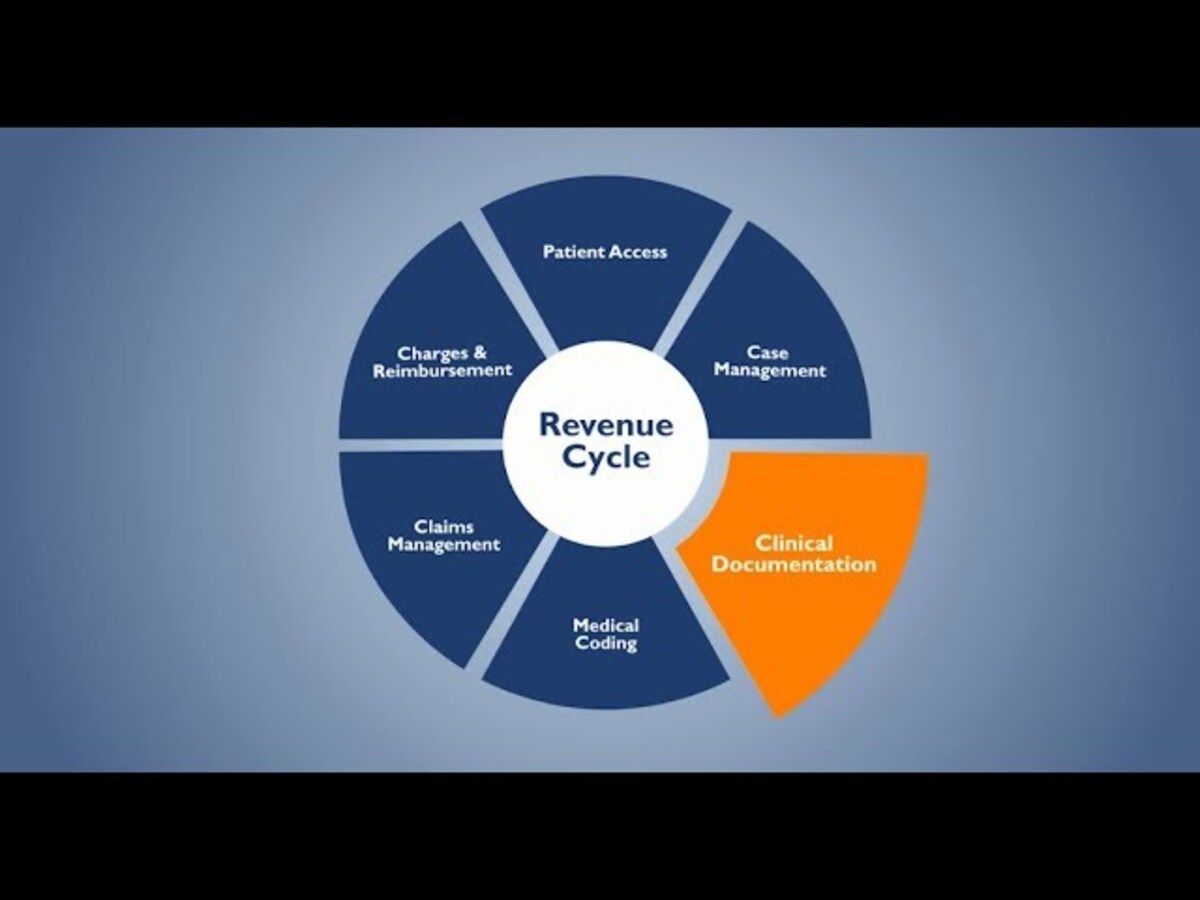
In the complex ecosystem of healthcare administration, the revenue cycle plays a pivotal role in ensuring the financial health and sustainability of healthcare organizations. From patient registration to reimbursement, the revenue cycle encompasses a series of interconnected processes aimed at capturing revenue for healthcare services rendered. In this blog post, we’ll delve into the key components of the revenue cycle in medical billing, shedding light on its stages, challenges, and importance in healthcare revenue management.
1. Patient Registration and Scheduling
The revenue cycle begins with patient registration and scheduling, where demographic and insurance information is collected, verified, and entered into the healthcare provider’s system. This initial step is crucial for establishing patient accounts, verifying insurance coverage, and determining eligibility for healthcare services.
2. Eligibility Verification and Pre-Authorization
Before providing medical services, healthcare providers must verify patients’ insurance coverage and obtain pre-authorization for certain procedures or treatments. Eligibility verification ensures that patients are covered for the services they receive and helps prevent claim denials and reimbursement delays.
3. Coding and Documentation
Once services are rendered, healthcare providers document the patient encounter, including diagnoses, procedures, treatments, and services provided. Medical coders then translate this clinical information into standardized codes, such as ICD (International Classification of Diseases) and CPT (Current Procedural Terminology) codes, which are used for billing and reimbursement purposes.
4. Claims Submission
After coding and documentation, claims are prepared and submitted to insurance companies, government payers, or third-party payers for reimbursement. Claims can be submitted electronically or via paper forms, along with supporting documentation, such as medical records and treatment notes.
5. Claims Adjudication
Upon receiving claims, insurance companies review them for accuracy, completeness, and medical necessity. Claims adjudication involves verifying patient eligibility, checking coverage benefits, and determining the amount of reimbursement owed to the healthcare provider. Insurers may approve, deny, or partially pay claims based on their coverage policies and reimbursement rules.
6. Payment Posting and Follow-Up
Once claims are adjudicated, payments are received from insurance companies, patients, or other payers. Payments are posted to the patient’s account, and any remaining balances are billed to the patient or secondary payers. Medical billing staff follow up on unpaid claims, resolve billing discrepancies, and appeal claim denials to ensure maximum reimbursement.
7. Patient Billing and Collections
Finally, patients are billed for any outstanding balances not covered by insurance. Patient statements are generated, detailing the services provided, insurance payments received, and patient responsibility. Healthcare organizations employ various methods to collect patient payments, such as payment plans, credit card processing, and debt collection agencies.
Importance of Revenue Cycle Management
Effective revenue cycle management is essential for healthcare organizations to optimize revenue, minimize financial losses, and maintain financial stability. By streamlining billing processes, reducing claim denials, and maximizing reimbursement, healthcare providers can improve cash flow, enhance operational efficiency, and focus on delivering quality patient care.
Conclusion
In conclusion, the revenue cycle is a multifaceted process that spans from patient registration to reimbursement and encompasses various stages and activities. Understanding the revenue cycle in medical billing is essential for healthcare providers to navigate the complexities of healthcare reimbursement, optimize revenue cycle management, and achieve financial success in today’s healthcare landscape. By adopting best practices, leveraging technology solutions, and prioritizing patient-centric billing practices, healthcare organizations can effectively manage the revenue cycle and ensure long-term financial sustainability.