In the intricate ecosystem of healthcare administration, maintaining financial stability is paramount for the sustainability and growth of healthcare organizations. At the heart of this endeavor lies revenue cycle management (RCM) – a strategic process designed to optimize the financial performance of healthcare providers by effectively managing the entire revenue cycle, from patient registration to payment collection. In this article, we explore the critical role of revenue cycle management in healthcare, its key components, and best practices for achieving operational excellence and financial health.
Understanding Revenue Cycle Management
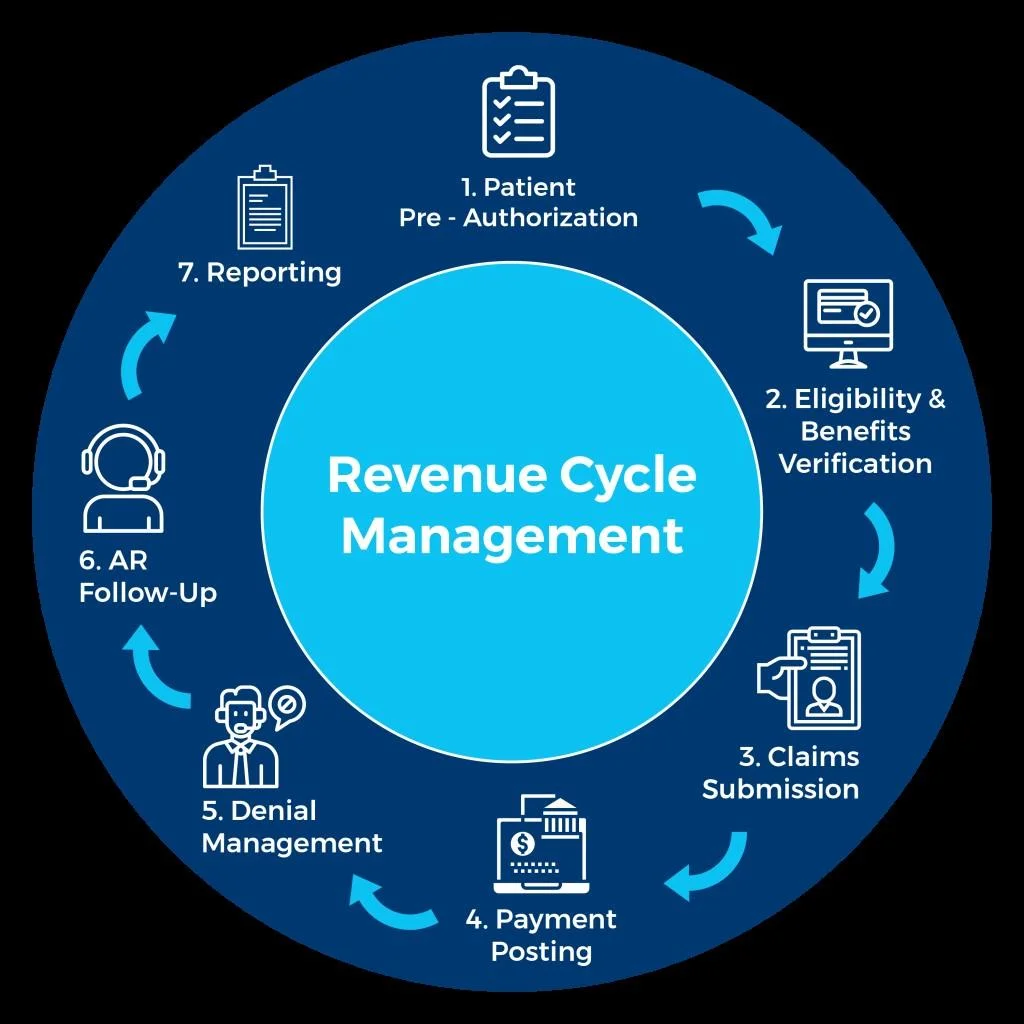
Revenue cycle management refers to the systematic process of managing healthcare providers’ financial transactions, from the moment a patient seeks medical services to the collection of payments for those services. This comprehensive approach encompasses a series of interconnected steps aimed at maximizing revenue, reducing inefficiencies, and enhancing the overall financial health of healthcare organizations.
Key Components of Revenue Cycle Management
- Patient Registration and Scheduling: The revenue cycle begins with the patient registration process, where accurate demographic and insurance information is collected. Effective scheduling practices ensure that appointments are optimized to maximize provider productivity and minimize patient wait times.
- Insurance Verification and Eligibility: Verifying patients’ insurance coverage and eligibility is essential to ensure timely reimbursement for services rendered. This step involves confirming insurance benefits, coverage limitations, and obtaining pre-authorization when necessary to avoid claim denials and billing discrepancies.
- Coding and Charge Capture: Accurate coding of medical procedures and services is critical for proper reimbursement. Healthcare providers must ensure that procedures are coded correctly using standardized code sets such as CPT, ICD-10, and HCPCS, capturing all billable charges associated with patient encounters.
- Claims Submission and Adjudication: Submitting clean claims to payers in a timely manner is essential for prompt reimbursement. Revenue cycle management involves monitoring claim status, identifying and addressing claim rejections or denials, and advocating for timely claim adjudication to optimize revenue flow.
- Patient Billing and Collections: Transparent and effective patient billing practices are key to facilitating payment and minimizing accounts receivable. Healthcare organizations must communicate clearly with patients regarding their financial responsibilities, offer convenient payment options, and implement robust collections strategies to recover outstanding balances.
- Denial Management and Appeals: Managing claim denials and appeals is a crucial aspect of revenue cycle management. Identifying the root causes of denials, implementing corrective measures, and pursuing appeals when necessary are essential for maximizing revenue recovery and reducing revenue leakage.
Best Practices for Revenue Cycle Management
- Streamlined Workflow and Technology Integration: Implementing integrated electronic health record (EHR) and practice management systems streamlines administrative processes, enhances data accuracy, and improves billing efficiency.
- Staff Training and Education: Investing in ongoing training and education for billing and administrative staff ensures proficiency in coding, billing regulations, and payer policies, reducing errors and enhancing compliance.
- Performance Monitoring and Analytics: Utilizing key performance indicators (KPIs) and analytics tools enables healthcare organizations to monitor revenue cycle performance, identify trends, and proactively address areas for improvement.
- Patient Engagement and Financial Counseling: Engaging patients early in the revenue cycle, providing transparent financial information, and offering financial counseling services can help prevent billing disputes and improve payment compliance.
- Continuous Process Improvement: Embracing a culture of continuous process improvement fosters innovation and efficiency in revenue cycle management. Regularly evaluating workflows, implementing feedback mechanisms, and adapting to industry changes are essential for optimizing financial performance.
Conclusion
In the ever-evolving landscape of healthcare, mastering revenue cycle management is essential for ensuring the financial health and sustainability of healthcare organizations. By adopting a comprehensive approach that encompasses patient registration, insurance verification, coding, claims submission, patient billing, and denial management, healthcare providers can optimize revenue flow, reduce costs, and enhance the overall patient experience. With strategic planning, technology integration, and a commitment to continuous improvement, healthcare organizations can navigate the complexities of revenue cycle management with confidence, achieving operational excellence and financial success in an increasingly competitive healthcare environment.